KNEE ARTHRITIS
Most of the knee pain experienced by the general population results from the normal wear and tear from aging. As we age the soft cushioning cartilage tissues hold less water reducing the amount of cushioning they provide and making them more susceptible to damage. Injury and auto immune issues can also play a role in destruction of the cartilage. We call the breakdown of cartilage arthritis and there are three basic types of arthritis that may affect the knee joint. Osteoarthritis, Rheumatoid Arthritis, and post-traumatic arthritis.
Types of Knee arthritis
Osteoarthritis
Osteoarthritis (OA) occurs most frequently. OA usually occurs slowly as a progressive degenerative disease in which the joint cartilage gradually wears away. It most often affects middle-aged and older people. Avascular necrosis of the knee can accelerate osteoarthritis and even cause young patients to require surgical intervention. Once enough of the cartilage has worn away bone rubs on bone causing pain and bone spurs that damage larger amounts of cartilage.
Rheumatoid Arthritis
Rheumatoid arthritis (RA) is an inflammatory type of arthritis that can destroy the joint cartilage. RA can occur at any age. RA generally affects both knees and other joints at the same time. Prompt treatment of RA can slow the progression of the disease and the unmerciful damage it inflicts on the body. While orthopedic surgeons may identify and diagnose RA, treatment of the condition requires another type of specialists called a Rheumatologist.
Post-traumatic Arthritis
Post-traumatic arthritis can develop after an injury to the knee. This type of arthritis presents the same as osteoarthritis and may develop years after a fracture, ligament injury, or meniscus tear. In post-traumatic arthritis the degradation of the joint initiates after an injury jump starts a cartilage degradation feedback loop leading to the progressive failure of the cartilage in the joint.
Symptoms of Arthritis
Generally, the pain associated with arthritis develops gradually, although sudden onset is also possible. The joint may become stiff and swollen, making it difficult to bend or straighten the knee. Pain and swelling are worse in the morning or after a period of inactivity. Pain and swelling may also increase after activities such as walking, stair climbing, or kneeling. The pain may often cause a feeling of weakness in the knee, resulting in a “locking” or “buckling.” Many people report that changes in the weather also affect the degree of pain from arthritis. Secondary issues may arise such as the formation of Baker’s cysts.
Treating knee arthritis
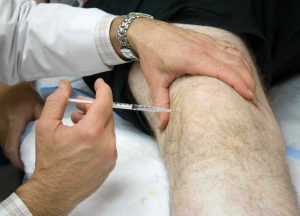 The first line of treatment for osteoarthritis includes a combination of non-steroidal anti-inflammatory drugs, or NSAIDs, for pain relief and to reduce the inflammation of the joint, along with education programs, wellness activities, and physical therapy. Patients with a BMI over 25 should participate in either a guided or self-guided weight loss program involving diet modification and low impact aerobic exercises. If first line conservative treatments fail to produce lasting relief then your provider may recommend injectable therapies aimed at increasing the hydration of the joint. Hyaluronic acid treatments called visco injections attract water molecules to help to lubricate the joint and reduce pain. Visco injections originally came from the comb of a rooster but due to allergic reactions they are mostly synthetic these days to reduce the chances of adverse reactions. For patients that respond to visco injections for a reasonable amount of time patients consider repeated injections over time to push back the need for joint replacement, but for patients that do not find acceptable relief will need an orthopedic surgeon consult to recommend a surgical intervention. Surgical interventions for knee arthritis include high tibial osteotomies in cases of young patients with medial single compartment osteoarthritis, unicomparmental arthroplasty for isolated compartment arthritis with intact ligaments, and total knee arthroplasty for cases that are not otherwise salvageable.
The first line of treatment for osteoarthritis includes a combination of non-steroidal anti-inflammatory drugs, or NSAIDs, for pain relief and to reduce the inflammation of the joint, along with education programs, wellness activities, and physical therapy. Patients with a BMI over 25 should participate in either a guided or self-guided weight loss program involving diet modification and low impact aerobic exercises. If first line conservative treatments fail to produce lasting relief then your provider may recommend injectable therapies aimed at increasing the hydration of the joint. Hyaluronic acid treatments called visco injections attract water molecules to help to lubricate the joint and reduce pain. Visco injections originally came from the comb of a rooster but due to allergic reactions they are mostly synthetic these days to reduce the chances of adverse reactions. For patients that respond to visco injections for a reasonable amount of time patients consider repeated injections over time to push back the need for joint replacement, but for patients that do not find acceptable relief will need an orthopedic surgeon consult to recommend a surgical intervention. Surgical interventions for knee arthritis include high tibial osteotomies in cases of young patients with medial single compartment osteoarthritis, unicomparmental arthroplasty for isolated compartment arthritis with intact ligaments, and total knee arthroplasty for cases that are not otherwise salvageable.

